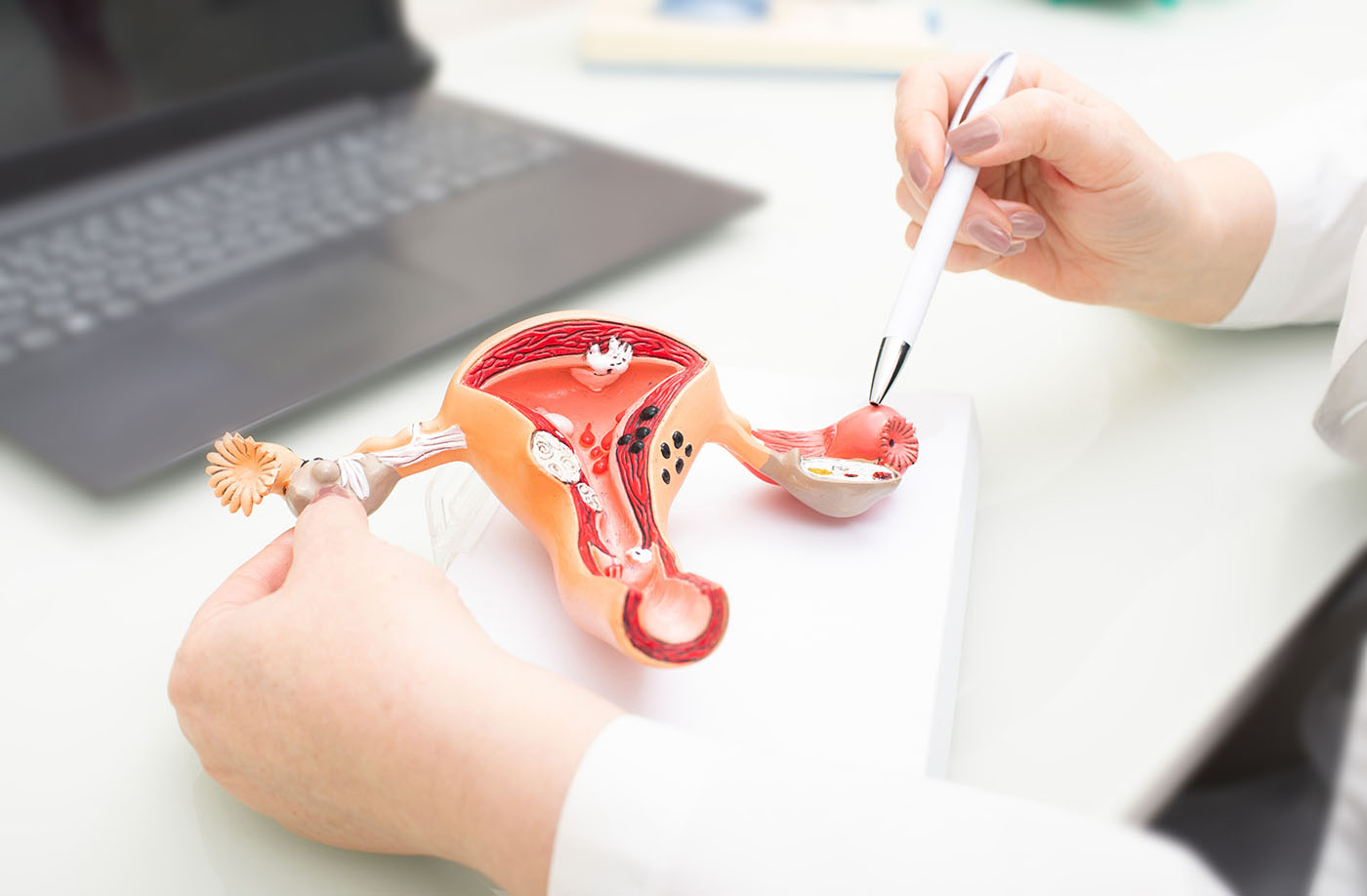
Ovarian insufficiency, also known as premature ovarian failure, occurs when your ovaries stop working properly before age 40. This can lead to reduced fertility, irregular or missed periods, and menopause-like symptoms such as hot flashes and mood swings. For women, this condition means facing challenges in conceiving naturally, and it can also affect your bone health and increase the risk of heart disease. Understanding and managing ovarian insufficiency is important for both your fertility and overall health.
Ovarian insufficiency affects women differently depending on their age. About 1 in 100 women under 40 experience it, while it’s less common in younger women—1 in 1,000 at age 30 and 1 in 10,000 at age 20. These numbers show that age plays a big role in the risk of developing this condition. It can also run in families, so if your mother or sister had it, you might be more likely to have it too.
Understanding the Triggers
Your egg supply and quality can decline for different reasons, making ovarian insufficiency more complicated. Some of these reasons are genetic, like Turner syndrome or Fragile X syndrome, which directly affect the number of eggs you have. Turner syndrome happens when a part of the X chromosome is missing, leading to symptoms like early ovarian failure. Fragile X syndrome, linked to the FMR1 gene, can also lower your egg count.
Other factors can also affect your eggs. Autoimmune diseases might attack your ovaries, interfering with normal egg production. Surgeries on the ovaries can reduce the number of healthy eggs by removing or damaging tissue. Cancer treatments like chemotherapy and radiation can harm the ovaries, reducing your egg supply. The extent of this damage depends on the type of treatment and your age.
Recognising and Diagnosing the Condition
You might discover you have ovarian insufficiency when looking into fertility issues. The hormonal changes can be subtle, especially if you’re younger, so it can be hard to detect without specific tests. Diagnosing ovarian insufficiency usually involves an ultrasound to count your follicles and blood tests to check hormone levels like FSH, oestradiol, and AMH. These tests help doctors understand how well your ovaries are working. Sometimes, more tests are needed to find out if genetic factors or previous treatments might be causing the condition.